Panic Disorder
Imagine you’re sitting in a quiet cafe in Melbourne, working through a few lines of code or planning a marketing launch, when suddenly, the air seems to vanish. Your heart isn’t just beating; it’s hammering against your ribs like a trapped bird. Your palms go cold and damp, and a wave of pure, unadulterated terror washes over you—despite the fact that you’re just sitting there with a latte.
For many, this is the terrifying introduction to a panic attack. But for those living with Panic Disorder, the attack itself is only half the battle. The other half is the “fear of the fear”—the persistent, looming anxiety that another attack could happen at any moment, in any place.
If you feel like your body has an overactive alarm system that triggers for no reason, you aren’t “losing it.” You are experiencing a manageable, biological misfire. Let’s break down the mechanics of the condition and look at practical, evidence-based Tips to Panic Disorder management to help you reclaim your sense of safety.
Panic Attack vs. Panic Disorder: Knowing the Difference
It is a common misconception that having a panic attack means you have Panic Disorder. In reality, up to 11% of adults will experience a panic attack in any given year, often triggered by extreme stress or a specific event.
Panic Disorder is diagnosed when these attacks become recurrent and unexpected. It’s defined by the persistent worry about having more attacks and the changes in behavior you make to avoid them. This often leads to agoraphobia—avoiding places where “escape” might be difficult, like elevators, public transport, or crowded shopping centers.
The Biology of a Misfire: Why It Feels So Real
To your brain, a panic attack is a success story. Your amygdala (the brain’s smoke detector) has sensed a threat and successfully triggered the fight-or-flight response. It floods your system with adrenaline, diverts blood to your muscles, and speeds up your breathing.
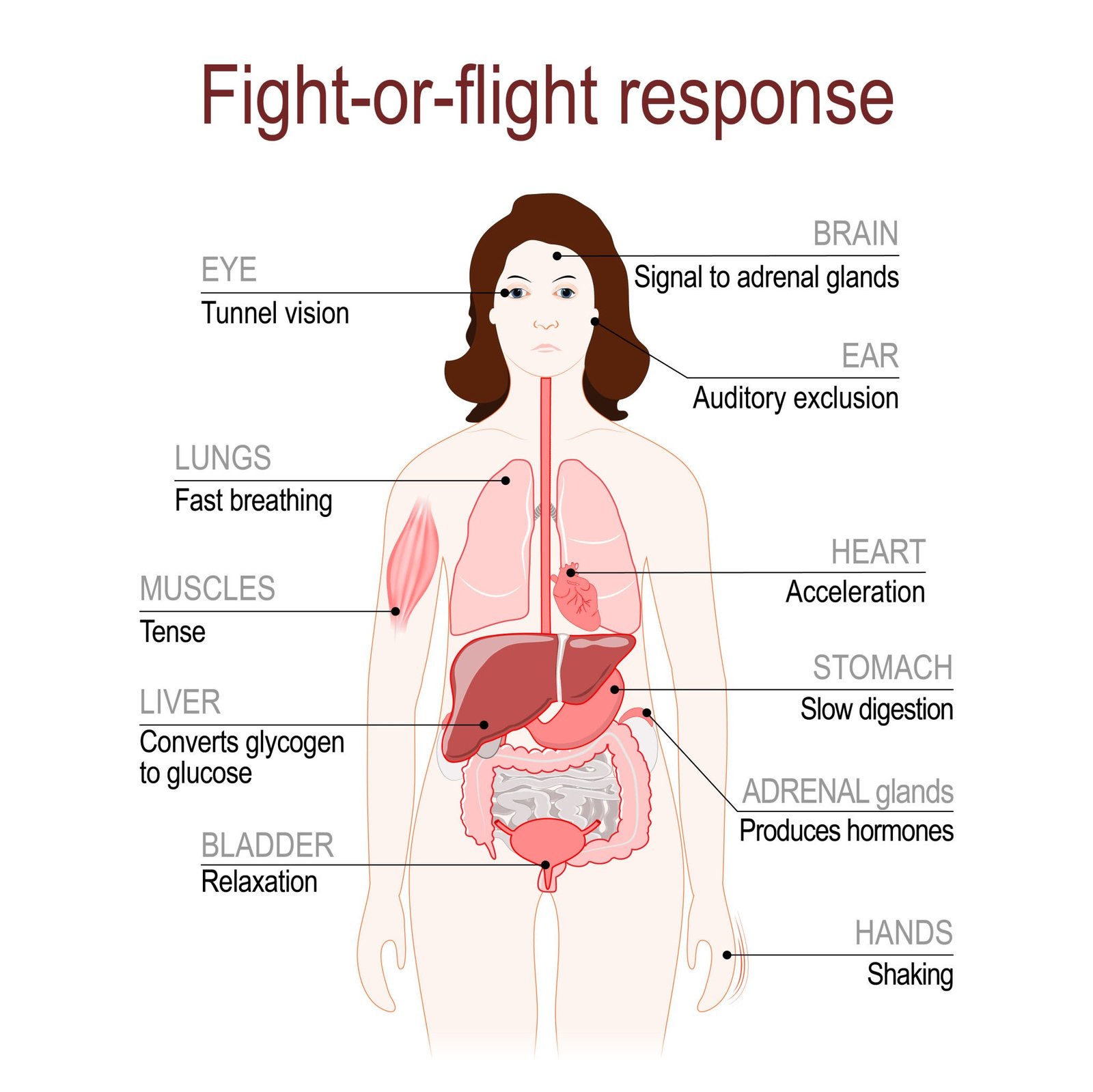
fight-or-flight response. stress response system.
he problem is that there is no tiger. Because there is no external threat to fight or run from, your brain tries to make sense of the physical sensations by creating a narrative: “I’m having a heart attack,” or “I’m going crazy.” These thoughts then feed back into the anxiety, creating a terrifying loop.

Essential Tips to “Panic Disorder” Recovery
Managing this condition isn’t about “wishing” the attacks away; it’s about retraining your nervous system to understand that it is safe. Here are the most effective Tips to Panic Disorder support.
1. The “Ride the Wave” Mentality
The natural instinct during an attack is to fight it. However, fighting a panic attack is like trying to fight a wave in the ocean—it just exhausts you and makes you feel more out of control.
- The Practice: Instead of resisting, practice “floating” through the sensations. Acknowledge them: “My heart is fast. My chest is tight. This is adrenaline. It is uncomfortable, but it is not dangerous.” Panic attacks typically peak within 10 minutes and then subside naturally. Let the wave break over you.
2. Interoceptive Exposure
This is a core component of Cognitive Behavioral Therapy (CBT). It involves intentionally inducing mild physical sensations that mimic panic in a safe environment to prove to your brain that they aren’t fatal.
- The Practice: Under the guidance of a professional, you might spin in a chair to feel dizzy or breathe through a straw to feel short of breath. By doing this repeatedly, you “habituate” to the sensations. You learn that dizziness is just dizziness—it doesn’t mean you’re going to faint.
3. The “Biological Anchor”
As we’ve discussed in our deep dives on [Magnesium for Anxiety] and [Vitamin D], your baseline chemistry matters. If your nervous system is already “brittle” due to deficiency or lack of sleep, the threshold for a panic attack is much lower.
- The Practice: Avoid high doses of caffeine and nicotine, which are stimulants that can “mimic” the start of a panic attack. Ensure you are getting adequate sleep to allow your amygdala to “recharge” and remain less reactive.
4. Grounding in the “Right Now”
When panic hits, your brain is in the future (“What if I die?”). Grounding pulls you back to the present.
- The Practice: Try the 5-4-3-2-1 Technique. Name 5 things you see, 4 things you can touch, 3 things you hear, 2 things you smell, and 1 thing you can taste. This forces the brain to shift from its “emotional” center back to its “sensory” center.
Addressing Common Concerns: “Is My Heart Okay?”
The most common fear during Panic Disorder is that the symptoms are actually a heart attack. While they feel remarkably similar, there are key differences. Panic symptoms usually include a racing heart and tingling in the hands, whereas a heart attack often involves a “crushing” pressure in the center of the chest and pain radiating to the arm or jaw.
If you’ve been to the ER and been given a clean bill of health, trust that data. Your heart is strong; it’s just receiving a “false alarm” from your brain.
The Path Forward: Professional Support
According to the National Institute of Mental Health (NIMH), Panic Disorder is highly treatable. CBT is considered the gold standard, often showing results in as few as 12 to 16 sessions. In some cases, medications like SSRIs are used as a “scaffolding” to help lower the baseline anxiety while you learn the coping skills necessary for long-term recovery.
Conclusion: Turning Off the Alarm
Living with Panic Disorder can make your world feel very small. You start avoiding the gym, the office, or your favorite restaurants because you’re afraid the “alarm” might go off. But remember: a panic attack is just a physical sensation. It is a surge of energy that has nowhere to go.
By applying these Tips to Panic Disorder, you are slowly teaching your brain that it can stand down. You are reclaiming the map of your life, one “scary” place at a time. You aren’t broken; your body is just trying to protect you a little too much. It’s time to let it know that you’ve got it from here.
Take the Next Step
- Subscribe to our newsletter for more evidence-based guides on mental resilience, digital wellness, and physical recovery.
- Leave a comment: What was the first “safe” place you reclaimed after a panic attack?
- Share this article: If you know someone who has been avoiding the world lately, send this their way. It might be the first step they need.









